The anatomy of “vaccine hesitancy,” and why it matters.
To solve it, we have to unpack what it means.
About 45% of Americans have received at least one dose of a COVID-19 vaccine. But the number of new vaccinations decreases daily—vaccine supply has eclipsed demand.
“Vaccine hesitant” is 2021’s term of art for the as-yet unvaccinated. However, I find the term unhelpful. Vaccine hesitancy masks all the variance in personal decisions (distrust, inaccessibly, dogmatic resistance) that are preventing us from reaching herd immunity.
Vaccine hesitancy is a catchall term that hides the variation underneath it.
Umbrella terms like “hesitancy” bury too much meaningful difference beneath them. So let’s step back and cut into what we mean by “vaccine hesitancy.”
There are, of course, the truly hesitant. To be “hesitant” is to be inclined, but with reservations. I might be hesitant to ride a roller coaster, or to try chocolate-covered ants, or to buy a pair of shoes that’s out of my price range. I want part of the thing, but I’m worried about some known or unknown consequence. The roller coaster would be a thrill—but what if my stomach can’t handle it? I love chocolate, just not ants. Though hesitant describes a particular subset of those who are as yet unvaccinated, as more of the hesitant are choosing to vaccinate, we have to be more specific about the motivations of those who remain unvaccinated.
Those include the vaccine resistant. Nearly 45% of Republicans say they will not get the vaccine. This tracks with an alarming trend that has aligned the Republican party with the anti-vaxxer movement. Donald Trump himself flirted with anti-vaxxers during his 2016 run for President. By 2020, he was the chief cheerleader of vaccines, as they were perhaps the only thing his administration did right vis-à-vis the pandemic. But he’s retreated back, refusing to publicly get the vaccine his own administration helped fund (though he was vaccinated on his way out of the White House).
Vaccine resistance is part of a broader trend among conservative populists toward denial of science as a means of ascertaining truth, as I’ve written about previously. Resisting vaccines amounts to dogma—right up there with COVID-19 denialism, making both particularly dangerous. That toxic brew has accounted for some of the country’s worst outbreaks in recent months.
Then there’s a difference between vaccine resistance and vaccine distrust. The latter do not deny science, but distrust that the scientists who perform it have their best interests in mind. What we call “vaccine hesitancy” among Black Americans often falls in this bucket. Experiences of discrimination by healthcare providers compounds decades of exploitation of Black people by the biomedical establishment. All of it casts doubt upon these vaccines developed in record time.
But there are yet others who are not hesitant, resistant, or distrustful, they simply lack vaccine urgency. For many of us, getting a vaccine was the most important thing we could possibly do—many put everything aside to hunt down an appointment. For others, it’s just not. Rather than hesitancy, which implies reservations, the vaccine non-urgent simply don't see getting vaccinated as a high priority among the many others in their lives. If they could get one without having to go out of their way, they would. But perhaps there’s just a lot in the way (as I wrote about in my last post). Or it just doesn’t seem worth going out of the way for because it’ll be available later when it’s more convenient. These tend to be younger people who don’t believe that they have high risk of disease.
Unpacking “hesitancy” helps us address it.
Distinguishing between types of non-vaccination matters because it disabuses us of the notion that there is somehow one solution to all “hesitancy.” What works for one group may not work for another.
For example, because of the high prevalence of vaccine resistance among political supporters of Donald Trump, there’s been some debate about whether or not a public call by him to take the vaccine would help. Focus group data from Republican pollster Frank Luntz showed that conservatives were more swayed by factual information from doctors than from GOP politicians. But Trump is singular among Republican politicians—given his cult-like control over the party and his supporters. His full-throated endorsement of the vaccine would likely have real impact among vaccine-resistant supporters.
But that might come at a cost for the vaccine distrustful, whose distrust may be stoked, in part, by the fact that the Trump administration had a hand in funding the vaccines. Instead, for the distrustful, it’s critical to build and amplify strong networks of validators from within their communities. Amplifying the voices of scientists and doctors of color is particularly critical.
What about the vaccine non-urgent? That comes back to the last mile problem I wrote about on Tuesday—make vaccines easier to get!
Incentives matter too.
Much of our focus on tackling “hesitancy” has been focused on messaging and trust. Those things, I believe, matter above all. It’s why I think it was critical that regulators chose to pursue a pause on the Johnson & Johnson vaccine when they found any hint of potential side effects that hadn’t been previously described. Though at the time, the potential impact on “vaccine hesitancy” became a subject of debate, the impact seems to have been minimal. Over time, I believe the wisdom of the pause will continue to grow.
But incentives matter too. In an op/ed about Michigan’s COVID-19 surge last month, I suggested:
Guidelines should be established that firmly tie activities allowed — traveling, going to the gym, eating in a restaurant — to specific vaccination rates. That would create the kind of benchmarks that both explain what the “right thing” is and incentivize public officials and the public to make it happen.
Incentives would assure that our haste to get back to the activities we’ve all missed doesn’t precede the safety of doing so. And second, it ties a vaccine decision to access to the things we want to get back to—whatever they may be—creating personalized incentives through collective policy.
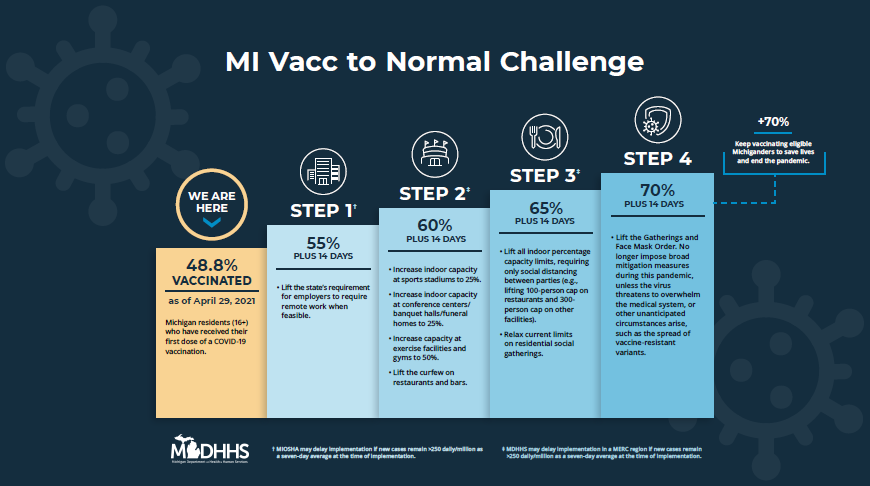
Last week, Governor Whitmer announced the “MI Vacc to Normal” campaign, which followed this incentive structure, tying reopening benchmarks to levels of vaccine.
Other states and companies have begun to offer incentives. Krispy Kreme is offering free donuts. The State of New Jersey is offering a free beer. West Virginia is offering a $100 savings bond!
Though in the end, the choice to get vaccinated comes down to trust and belief in science and scientists, incentives matter because they change the benefit structure on the other side of getting vaccinated. And in the end, everyone loves a donut...well, most people, anyway.





I love how you unpacked what vaccine hesitancy means. This is all so true. As a family doctor, it is challenging for me to find time to discuss getting a COVID-19 vaccine with my patients, but I try my best to do it anyway. I always make sure that I discuss all my patients' concerns before I drop that big question, "have you considered or have you taken the COVID-19 vaccine?" (I have changed it from "have you scheduled or taken the COVID-19 vaccine because there have been times when I had gotten violent reactions from asking) I think even if they are very resistant to getting vaccinated, patients are more open to listen when they have seen that I have already worked on gaining their trust by addressing their health concerns. I always try to lighten up the conversation by sharing my personal experience with the vaccine or how I had a 100+ year old patient who got the vaccine, got a rash and felt bad, but she survived. I always ask everyone who have been vaccinated if they had any side effects because I tell those who are hesitant that "I ask everyone who has gotten it and I can promise you that at least 95% had no to minor side effects." I guess the next question is how can I make my patients trust science again, because that's the hardest one for me, when they believe that it has not been studied long enough. Because science always wins, right? But we have to convince a lot of people first.